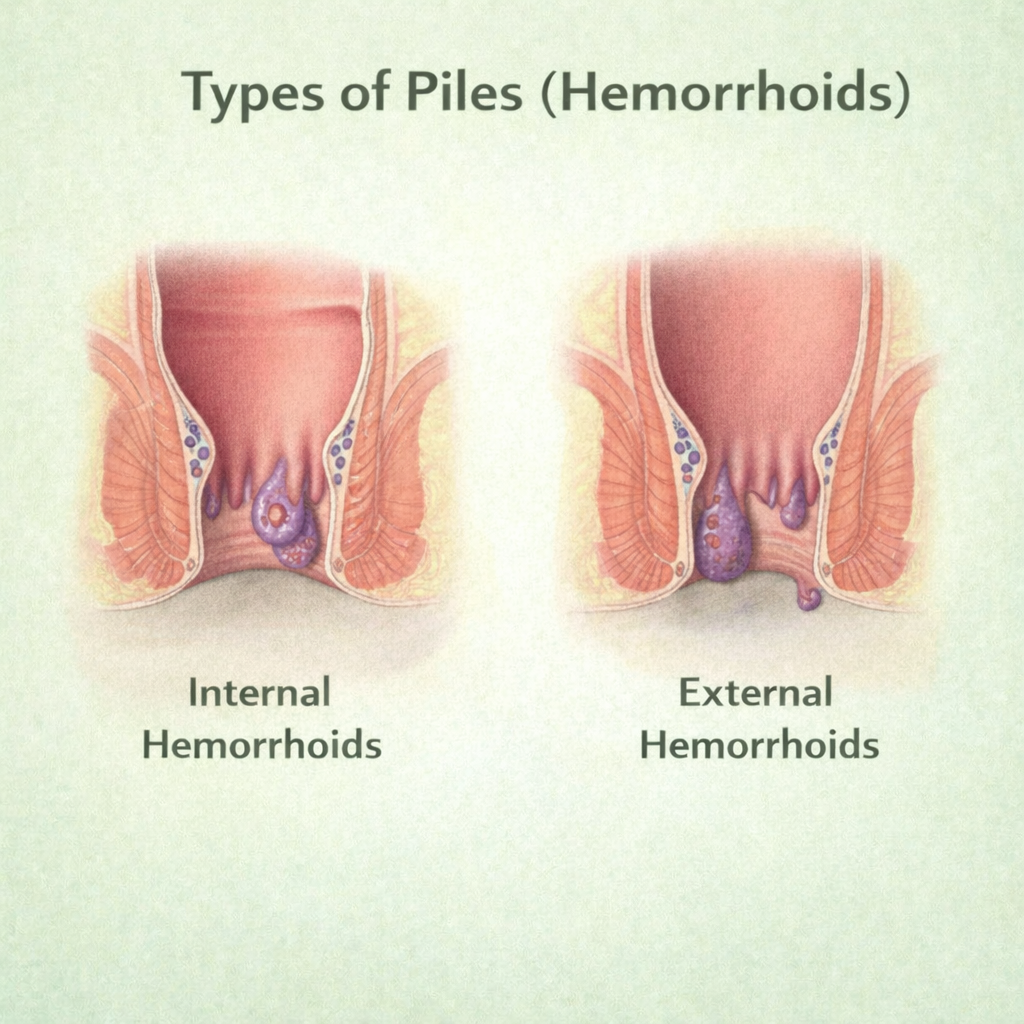
What are Piles (Hemorrhoids)?
Piles, medically known as hemorrhoids, are swollen and inflamed veins in the rectum and anus, similar to varicose veins. They develop when increased pressure stretches the blood vessels, causing them to bulge. Hemorrhoids can be:
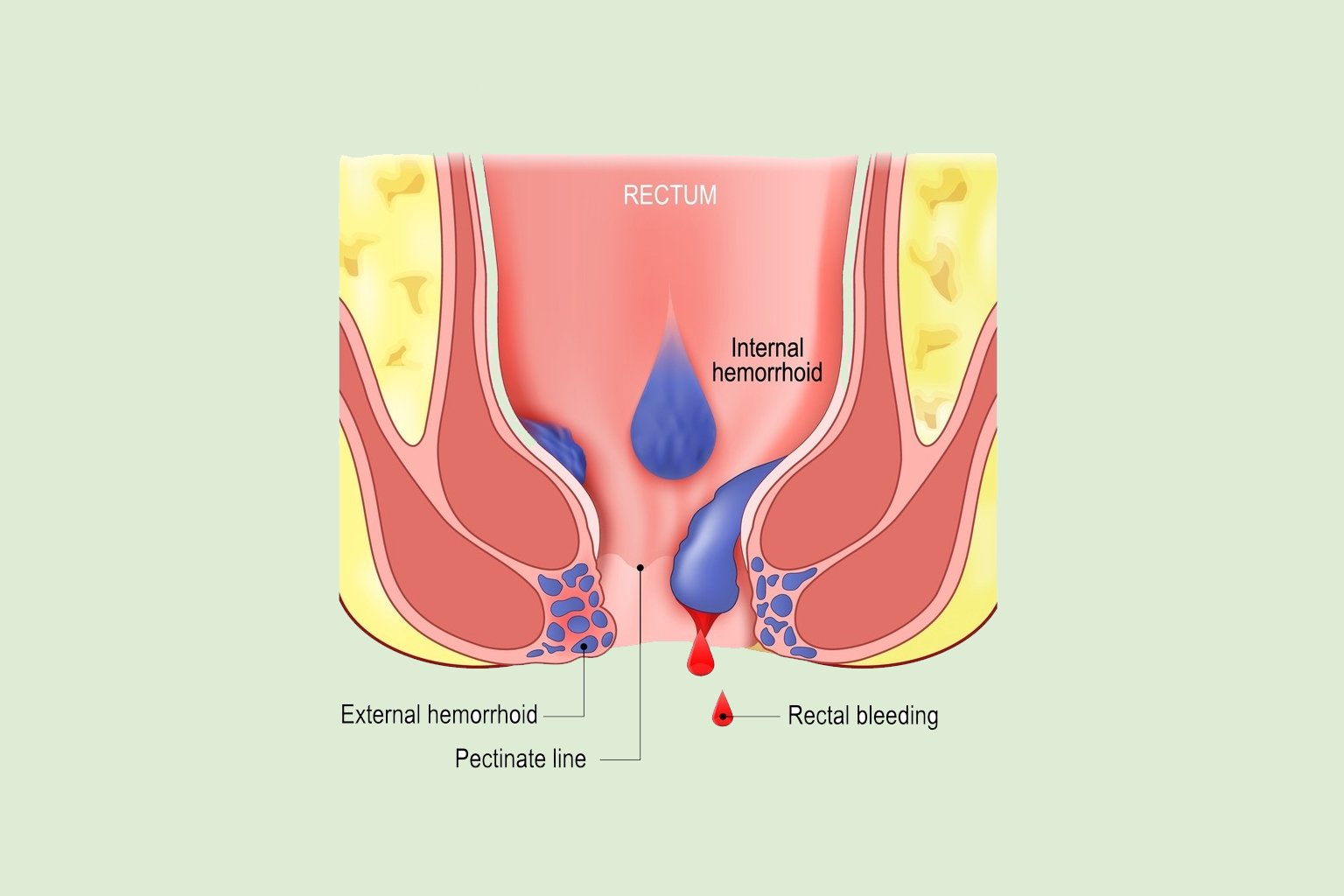
Internal Hemorrhoids: Occur inside the rectum
External Hemorrhoids: Occur under the skin around the anus
Hemorrhoids are extremely common, affecting about 50% of adults by age 50.
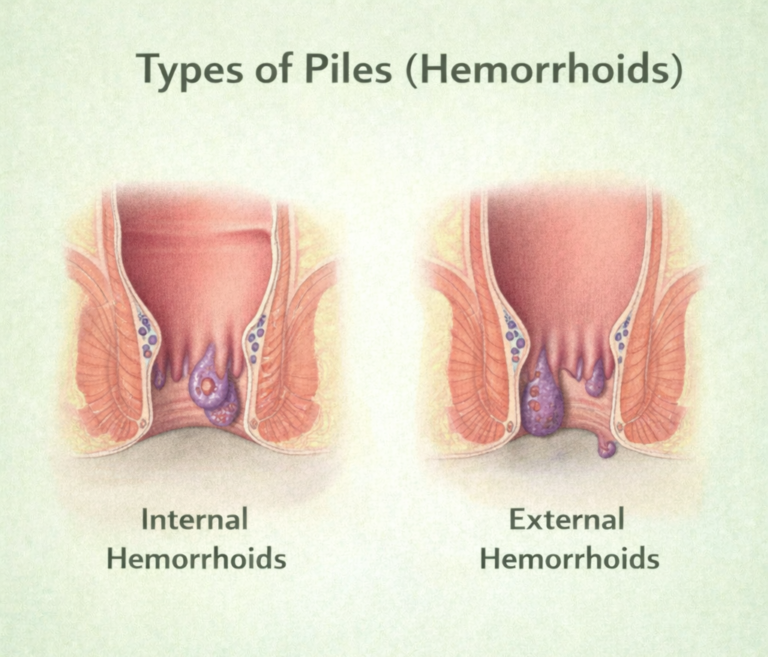
Grades of Internal Hemorrhoids
Grade 1: Small, inside anal canal, may bleed
Grade 2: Protrude during bowel movements but return inside on their own
Grade 3: Protrude and need manual pushing back
Grade 4: Permanently prolapsed, cannot be pushed back; may become strangulated
External hemorrhoids may form thrombosed lumps (blood clots) that are painful.
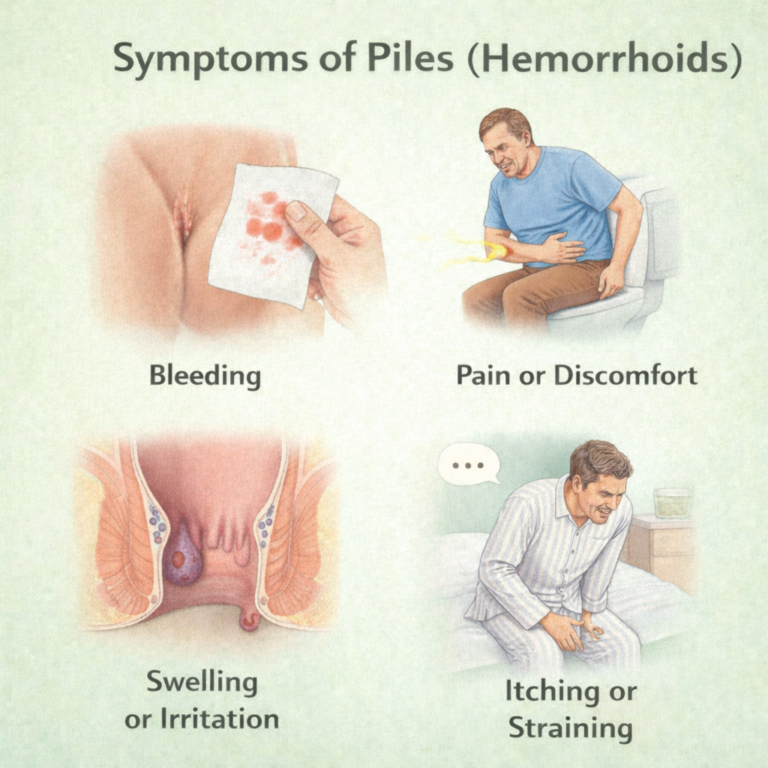
Symptoms of Piles
Bright red blood on toilet paper or in stool
Itching or irritation around the anus
Pain or discomfort during bowel movements
Lumps or swelling near the anus
Leakage of feces or mucus
Feeling of incomplete bowel evacuation
Prolapsed tissue visible outside the anus
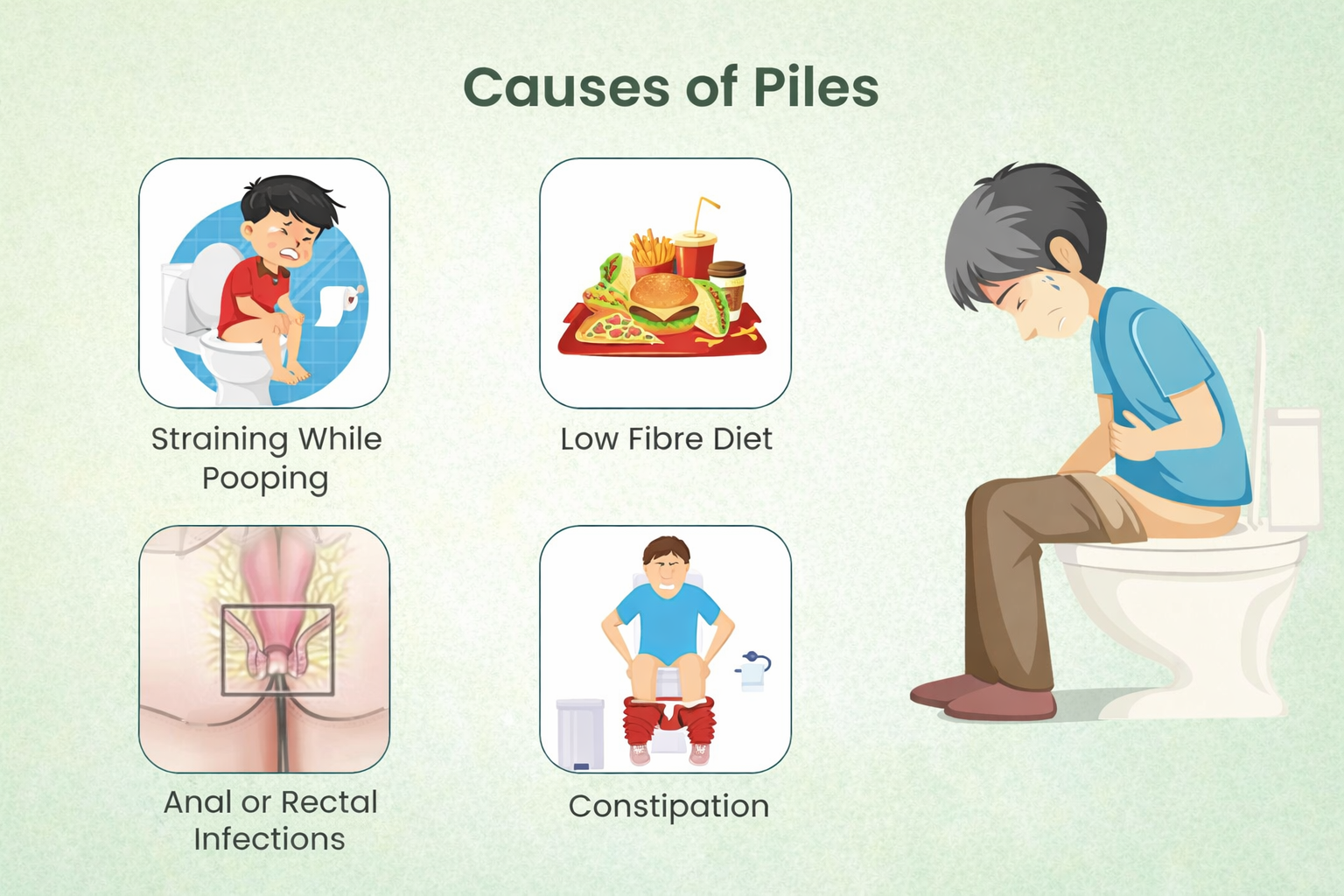
Causes of Hemorrhoids
Bright red blood on toilet paper or in stool
Itching or irritation around the anus
Pain or discomfort during bowel movements
Lumps or swelling near the anus
Leakage of feces or mucus
Feeling of incomplete bowel evacuation
Prolapsed tissue visible outside the anus
Prevention Tips
Eat a high-fiber diet (fruits, vegetables, whole grains)
Drink 8–10 glasses of water daily
Exercise regularly to prevent constipation
Avoid straining and prolonged sitting on the toilet
Go to the bathroom as soon as you feel the urge
Maintain a healthy weight
Practice good hygiene and avoid heavy lifting

Risk Factors
Chronic constipation or diarrhea
Low-fiber diet
Age over 50 (weakened tissues)
Pregnancy and childbirth
Obesity
Sedentary lifestyle or prolonged sitting
Anal intercourse
Liver disease or portal hypertension
Family history of hemorrhoids

Modern Treatment Advantages
Multiple treatment options tailored to severity
Minimally invasive techniques available
Laser and Doppler-guided procedures reduce pain and recovery time
High success rates with modern approaches
Proper hemorrhoid management can relieve pain, restore normal bowel function, and significantly improve quality of life. Early consultation ensures the best treatment option, whether conservative, minimally invasive, or surgical.

When to See a Doctor
Emergency: Severe pain or large amounts of rectal bleeding
Consultation: Bleeding lasting more than a week, dark/tarry stool, persistent symptoms not relieved by home care, severe pain not responding to over-the-counter treatments, or first-time bleeding after age 40
Seek immediate medical attention for severe pain or large amounts of rectal bleeding. Schedule a doctor's visit if you have rectal bleeding lasting more than a week, blood in stool appears dark or tarry, hemorrhoid symptoms don't improve with home treatment after a week, severe pain not relieved by over-the-counter treatments, symptoms interfere with daily activities, or you're over 40 experiencing first-time rectal bleeding (to rule out other conditions). Most hemorrhoids respond to conservative treatment including fiber supplements, stool softeners, warm baths, and topical treatments. Persistent or severe cases may require procedures like rubber band ligation, sclerotherapy, or surgical removal.